Ureteroscopy for kidney stone disease
CONDITIONS
Written and Medically Reviewed by Mr Ivo Dukic, Consultant Urologist | Last updated: 15/03/2026
Private ureteroscopy in Birmingham
Ureteroscopy (URS) is a minimally invasive medical procedure used primarily to locate and treat stones within the urinary tract. Because it utilises the body's natural pathways, no surgical incisions are required. A urologist gently inserts a highly flexible, ultra-thin tube called a ureteroscope—which is equipped with a light and a high-definition camera—through the urethra, into the bladder, and up into the ureter or kidney. Once the stone is directly visualised on a monitor, the surgeon can pass tiny specialised instruments through the scope, such as a laser fibre to break the stone into fine dust or a delicate wire basket to capture and extract the pieces. This allows for the precise removal of the stones with a relatively rapid recovery time compared to traditional surgeries.
When is Ureteroscopy Recommended?
Ureteroscopy (URS) is a procedure used to treat kidney or ureteric stones that are causing severe symptoms or are unlikely to pass on their own. Medical guidelines, including those from NICE, typically recommend this procedure in the following scenarios [1]:
Persistent Pain: When conservative management (waiting for the stone to pass naturally) fails to relieve ongoing pain. [1]
Blockage (Obstruction): When a stone blocks the urinary tract, which can potentially damage the kidney if left untreated.
Infection: If a stone is linked to a urinary tract infection, it must be removed quickly to prevent complications. This may initially require placing a temporary drainage tube (a stent or nephrostomy). [1,2]
Ineffective Medication: When drugs designed to help pass the stone do not work. [1]
Stone Size and Location: The likelihood of a stone passing naturally depends heavily on its size. Data shows that 5–7 mm stones have about a 60% chance of passing on their own. This drops to 48% for 7–9 mm stones, and only 25% for stones over 9 mm. Stones larger than 10 mm rarely pass naturally [3]. For stones between 10–15 mm, guidelines recommend URS as the primary surgical option, while larger or more complex stones (over 20 mm) may require a more invasive keyhole surgery (PCNL). [1,2,4]
The Benefits of Ureteroscopy
Compared to other treatments, ureteroscopy offers several distinct advantages:
High Success Rates: Recent data from a large study of over 6,400 cases shows real-world success rates (meaning no stones remain, as confirmed by CT scans) of roughly 50% for kidney stones and 73% for stones in the ureter [5]. Success rates can range up to 90% depending on the surgeon, stone size, and location [5]. When using newer equipment with suction technology, success rates have been reported as high as 92.9–95% [7]. It also consistently outperforms shockwave therapy (SWL) in comparative studies [6].
Minimally Invasive: The doctor uses a thin, flexible camera inserted through the body's natural pathways. There are no incisions, which minimises tissue damage and speeds up recovery.
Immediate Relief: Patients generally experience fast relief from pain and blockages right after the procedure.
Versatile: It is highly effective for treating stones of various sizes and locations. Guidelines confirm it generally requires fewer repeat treatments than shockwave therapy [8].
Diagnostic Value: Because it uses a camera, doctors can directly inspect the urinary tract to identify any other potential issues.
Comparing Stone Treatments: ESWL, URS, and PCNL
When deciding how to remove a stone, urologists typically choose between three main procedures based on the stone's size, location, and makeup.
Shockwave Therapy (ESWL): A non-invasive outpatient procedure using targeted sound waves from outside the body to break the stone into fragments, which the patient then pees out over several weeks.
Ureteroscopy (URS): A minimally invasive procedure where a small camera is passed through the urinary tract to find the stone, break it with a laser, and remove the pieces.
Keyhole Surgery (PCNL): A procedure for very large or complex stones that requires a small incision in the back to access the kidney directly.
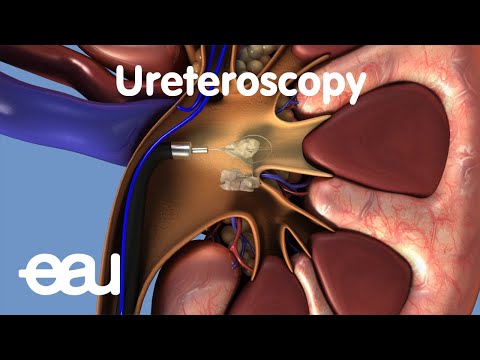
Technological Advancements: Suction Sheaths
A major recent upgrade to ureteroscopy is the use of "suction access sheaths." Normally, a protective tube (sheath) is placed in the ureter to allow the camera to slide in and out safely. Newer versions of these tubes now feature a built-in vacuum mechanism, offering significant clinical benefits:
Clearer Visibility: The vacuum continuously removes stone dust and minor bleeding created by the laser, giving the surgeon a crystal-clear view of the operating area. [15,16]
Better Stone Removal: Instead of relying on the surgeon to manually fish out tiny pieces with a wire basket—or leaving dust for the patient to pass—the vacuum automatically removes fragments as they are created. Studies show this leads to near-perfect immediate clearance rates (up to 96.5% for single kidney stones) and reduces the need for post-surgery stents. [7,17]
Lower Kidney Pressure (Safer Procedure): To see clearly, fluid is continuously pumped into the kidney during surgery. This can increase internal pressure, risking fluid absorption into the bloodstream and causing post-surgery infections. The vacuum safely pulls this fluid out, keeping pressure low and significantly reducing the risk of infection. [15,16,18]
Laser stone surgery — Thulium in Birmingham
The most significant recent advance in laser stone surgery is the introduction of the Thulium fibre laser (TFL), which represents a genuine step forward from older Holmium lasers that have been the standard for the past two decades. The Thulium laser operates at a higher pulse frequency. It delivers energy more efficiently, which means it can reduce even hard kidney stones to an extremely fine dust — so fine that the fragments often don't need to be physically retrieved at all. This "dusting" approach is not just a technical nicety; it translates directly into better stone clearance rates and fewer repeat procedures for patients. Where Thulium laser technology becomes particularly powerful is in combination with the latest suction access sheath systems. The vacuum mechanism built into these sheaths continuously removes stone dust and fluid as the laser works, keeping the operative field clear and — crucially — preventing the fine particles from scattering to inaccessible parts of the kidney. Together, Thulium laser and suction sheath technology represent the current gold standard in flexible ureteroscopy, and both are available as part of our kidney stone surgery service in Birmingham.
Risks and Limitations of Ureteroscopy
While generally safe and routine, ureteroscopy does carry some risks:
Infection: There is a 5–10% chance of developing a urinary tract infection after the procedure, which may require antibiotics. [19] Severe complications are rare (1.5–2.9%). [10]
Bleeding: Minor bleeding in the urine is expected, but severe bleeding is uncommon.
Injury to the Ureter: The scope can sometimes scratch or injure the urinary tract (1–2% of cases) [19, 20]. Very rarely (1 in 2,000 to 4,000 procedures), this might require open surgery to repair. [20]
Stone Movement: Stones may accidentally shift to a harder-to-reach location during the surgery.
Remaining Stones: It is relatively common that not all stone fragments are cleared, especially in the kidney. Real-world data shows a 50% total clearance rate for kidney stones versus 73% for ureter stones. Larger stones or those in tricky locations are harder to clear entirely. [5]
Stent Discomfort: Most patients require a temporary internal tube (stent) after surgery. These commonly cause discomfort, abdominal pain, a frequent urge to pee, and minor bleeding, which can temporarily affect a patient's ability to work. [13,21]
Anaesthesia Risks: As with any surgery requiring general anaesthesia, there are baseline risks, especially for patients with other health conditions.
Note: Further patient information on kidney stones and procedure risks can be found via the British Association of Urological Surgeons and through the European Association of Urology.
Following the procedure:
Remember, successful stone management extends beyond the procedure itself:
Hydration: Aim for 2.5 -3 litres of water daily to prevent or delay further stone formation.
Dietary modifications: Minimise stone-forming foods like animal protein and oxalates based on your stone type.
A ureteric stent is often inserted with some removal strings which come outside the urethra. The ureteric stent is often removed 3-5 days following a ureteroscopy operation. In some cases a ureteric stent can be left in for a few weeks to allow healing of a ureter if there are problems during your procedure. For these patients a further procedure where a flexible camera is inserted under local anaesthetic into the bladder is required to remove the ureteric stent.
Scheduled check-ups can ensure timely detection and management of any recurrent stones if required.
After surgery, if you are having ongoing pain, urinary tract infections of blood in the urine please get in contact with your surgeon so that we can organise further imaging tests (usually a CT scan) to look for any problems following the surgery.
This article provides general information and should not substitute for professional medical advice that is tailored to your situation with your urologist. Always consult a urologist for a personalised assessment and treatment plan.
The specific risks and benefits of ureteroscopy may vary depending on individual circumstances and your exact presentation.
Mr Ivo Dukic is regarded as one of the leading kidney stone surgeons in the UK, combining vast surgical experience in kidney stone surgery with a patient-centred approach from his base in Birmingham, West Midlands. His practice is a destination for patients seeking definitive treatment for all types of kidney stone disease.
Why Patients Choose Mr Dukic for their kidney stone surgery:
Expert in Complex Kidney Stone Surgery: Possesses the specialist skill required to manage large, complex, and recurrent kidney stones that other surgeons may not be equipped to treat.
High-Volume PCNL Surgeon: As a high-volume surgeon, he performs a significant number of PCNL procedures annually, a key indicator of proficiency and one of the reasons he is considered amongst the best kidney stone surgeons in the UK.
Pioneer in Minimally Invasive Treatment: Utilises the most advanced, state-of-the-art techniques, including supine PCNL, mini-PCNL and ultra-mini PCNL, to minimise patient recovery time and improve surgical outcomes.
Accessible Across the UK: Based in centrally located Birmingham, West Midlands, he treats patients who travel from across the United Kingdom and internationally for his specialist care.
Rapid Access for Urgent or Ongoing Problems: Whether you are struggling with the discomfort of a ureteric stent, experiencing recurrent pain, urinary tract infections, or blood in the urine related to a kidney stone, or simply facing a lengthy NHS waiting list for surgery, Mr Dukic offers rapid-access appointments — typically within 7 days — so that your symptoms are assessed and a clear treatment plan is in place without delay.
You can schedule an appointment with him for expert, bespoke advice through his Top Doctors profile or book an appointment through Harborne Hospital, HCA Healthcare, the Priory Hospital, Edgbaston, Circle Health Group, Droitwich Spa, Circle Health or Spire Parkway, Solihull.
Frequently Asked Questions About Private Ureteroscopy in Birmingham
How long does ureteroscopy take and will I need to stay overnight?
Most flexible ureteroscopy procedures take 30–90 minutes, depending on stone size and location. The majority of patients are discharged the same day, within a few hours of waking from anaesthetic. Patients with larger stone burdens or who have had a more complex procedure occasionally stay overnight.
Will I need a stent after ureteroscopy?
A ureteric stent is placed in most cases at the end of ureteroscopy to allow the kidney to drain freely while post-operative swelling settles. In Mr Dukic's practice, stents are routinely placed with attached strings for home removal at 5–7 days. For suitable patients with uncomplicated ureteric stones, stentless ureteroscopy — with no stent at all — is offered. Discuss this preference at your consultation.
How is the stent removed after ureteroscopy?
Mr Dukic routinely uses stents with an attached string that exits through the urethra. The string allows removal at home by the patient (using gentle, steady traction) or by a nurse, without a further clinical procedure or visit to the endoscopy suite in most cases. This is arranged for 3–7 days post-operatively.
What is the difference between Thulium and Holmium laser for kidney stones?
Holmium:YAG laser has been the standard for ureteroscopy for over two decades. Thulium fibre laser is the newer generation, converting stones into fine powder (dusting) rather than fragments, with less tendency to push stones backwards during treatment (retropulsion). In practice, Thulium achieves stone-free status more often in a single procedure and performs better on most stone compositions. Mr Dukic uses Thulium fibre laser as standard where available.
What is the success rate for ureteroscopy?
Stone-free rates for ureteroscopy depend significantly on stone size, location, and composition. For ureteric stones up to 1 cm, single-procedure stone-free rates are typically 85–95%. For kidney stones up to 2 cm, rates are approximately 70–90% depending on stone characteristics. Mr Dukic will discuss the realistic expected outcome for your specific stone at your pre-operative consultation.
Can I have ureteroscopy if I'm already on an NHS waiting list?
Yes. Private ureteroscopy does not affect your NHS waiting list position. Many patients choose to proceed privately to avoid waiting with a stent in situ, then cancel their NHS listing once treated.
How much does private ureteroscopy cost in Birmingham?
The initial consultation is £300. Surgical fees for ureteroscopy vary by hospital and stone complexity but UK private ureteroscopy generally ranges from approximately £6,000–£9,000. Mr Dukic is fully fee-assured with BUPA, AXA PPP, Aviva, Vitality, WPA, Cigna, AIG and Aetna. Self-pay pricing is confirmed in writing before you commit to surgery.
Do I need a referral to book a private ureteroscopy consultation?
No. You can self-refer by calling 0121 716 9046 or booking online. Existing imaging (CT KUB, CT urogram) and any referral letters are very helpful — please bring these to your consultation.
References
National Institute for Health and Care Excellence (NICE). Renal and ureteric stones: assessment and management. NICE guideline [NG118]. London: NICE; 2019 [updated 2019 Jan]. Available from: https://www.nice.org.uk/guidance/ng118
European Association of Urology (EAU). EAU Guidelines on Urolithiasis. Arnhem: EAU; 2024. Available from: https://uroweb.org/guidelines/urolithiasis
Coll DM, Varanelli MJ, Smith RC. Relationship of spontaneous passage of ureteral calculi to stone size and location as revealed by unenhanced helical CT. AJR Am J Roentgenol. 2002;178(1):101-3.
Getting It Right First Time (GIRFT). Towards better care for patients with acute urinary tract stones. London: GIRFT; 2021. Available from: https://www.gettingitrightfirsttime.co.uk
Jain R, Sagu A, Tiselius HG, et al. Real-world CT-assessed stone-free rates for ureteroscopy: a multicentre cohort of 6,487 cases. Eur Urol Focus. 2023.
Jain R, Sagu A, Tiselius HG, et al. Propensity-matched comparison of shockwave lithotripsy and ureteroscopy for renal and ureteral stones. Clin Kidney J. 2018.
Gauhar V, Somani BK, et al. Stone-free rates with single-use ureteroscopes and suction access sheaths: 30-day CT follow-up. Sci Rep. 2025.
Somani BK, et al. International Alliance of Urolithiasis (IAU) guideline on retrograde intrarenal surgery. BJU Int. 2023.
National Institute for Health and Care Excellence (NICE). Renal and ureteric stones: assessment and management. Evidence review B: Imaging for diagnosis. NICE guideline [NG118]. London: NICE; 2019. Available from: https://www.nice.org.uk/guidance/ng118/evidence
British Association of Urological Surgeons (BAUS). BAUS 2020 Meeting Abstracts. J Clin Urol. 2020;13(1S). Available from: https://www.baus.org.uk
International Surgery Journal. Influence of stone burden and stone configuration on outcomes of percutaneous nephrolithotomy. Int Surg J. 2016;3(1):195-200.
Abdel-Razzak OM, Alhazmi HM. Extracorporeal shock wave lithotripsy vs ureteroscopic lithotripsy for impacted ureteric stones. Urol Ann. 2013;5(3).
Joshi HB, Stainthorpe A, MacDonagh RP, Keeley FX Jr, Timoney AG, Barry MJ. Indwelling ureteral stents: evaluation of symptoms, quality of life and utility. J Urol. 2003;169(3):1065-9.
de la Rosette J, Assimos D, Desai M, et al. The Clinical Research Office of the Endourological Society Percutaneous Nephrolithotomy Global Study: indications, complications, and outcomes in 5803 patients. J Endourol. 2011;25(1):11-7.
Chen Y, Li C, Gao L, et al. Novel flexible vacuum-assisted ureteral access sheath can actively control intrarenal pressure and obtain a complete stone-free status. J Endourol. 2022;36(9):1143-8.
Li C, Chen Y, et al. Comparison between flexible and navigable suction ureteral access sheath and conventional ureteral access sheath in retrograde intrarenal surgery. BMC Urol. 2025;25:47.
Somani BK, Gauhar V, et al. Flexible And Navigable Suction ureteral access sheath (FANS): global multicentre prospective study with CT-assessed outcomes. Presented at: BAUS Annual Scientific Meeting 2024; Manchester, UK.
Li J, et al. Tip-bendable suction ureteral access sheath for retrograde intrarenal surgery: reduced intrarenal pressure and improved stone clearance. BMC Urol. 2025.
De Coninck V, Keller EX, Somani BK, et al. Complications of ureteroscopy: a complete overview. World J Urol. 2020;38(9):2147-66.
British Association of Urological Surgeons (BAUS). National audit of ureteric injuries during urological procedures. BAUS Annual Report 2022-2023. London: BAUS; 2023. Available from: https://www.baus.org.uk
British Association of Urological Surgeons (BAUS). Procedure-specific patient information: ureteroscopy and stone fragmentation. London: BAUS. Available from: https://www.baus.org.uk/patients/procedures
Have any questions?


If you have any questions or wish to make an appointment please get in contact.
Ivo Dukic
Contacts
e-mail: admin@ivodukic.co.uk
Telephone number for private patients:
0121 716 9046
(Mondays to Fridays 0800 - 18:00)
For NHS patients seen at University Hospitals Birmingham NHS Hospitals please get in contact on
0121 424 9011
(Mondays to Fridays 0900 - 17:00)
ivodukic.co.uk
© 2026 UrolSurg LTD
GMC 6103172
BSc MBChB PG Cert FRCSEd (Urol)


